The Silent Epidemic: Why Misdiagnosing Sleep Disorders Puts Health at Risk
Sleep is not merely a luxury; it's a fundamental pillar of our health and well-being. Yet, for millions worldwide, restful sleep remains an elusive dream. Sleep disorders, encompassing everything from chronic insomnia to sleep apnea, are a silent epidemic with far-reaching consequences. What’s even more alarming is the often-poor diagnostic process that frequently leads to questionable medication prescriptions, potentially masking serious underlying issues and creating new health risks. This critical situation highlights a significant gap in healthcare, where the complexities of what might be termed an
Lfs Krankheit – a sleep-related illness often characterized by diagnostic ambiguity – are frequently underestimated.
The Far-Reaching Impact of Undiagnosed Sleep Disorders
The repercussions of chronic sleep disturbances extend far beyond just feeling tired. When the body and mind are deprived of restorative sleep, the domino effect on health is profound and pervasive.
*
Physical Deterioration: Persistent sleep deprivation significantly impacts physical conditioning. Individuals may experience chronic fatigue, reduced cognitive function, weakened immune systems, and an increased risk of accidents. Over time, it can contribute to a host of serious physical ailments, including cardiovascular disease, diabetes, and obesity.
*
Strained Social Relationships: The irritability, mood swings, and lack of energy associated with poor sleep can severely strain personal and professional relationships. Difficulty concentrating and engaging in social activities can lead to isolation and further exacerbate emotional distress.
*
Mental and Emotional Health Crisis: Perhaps one of the most concerning links is the elevated risk of psychosomatic illnesses, depression, and neuroses. Sleep disorders often co-exist with mental health conditions, creating a vicious cycle where each exacerbates the other. An undiagnosed
Lfs Krankheit can thus pave the way for a deteriorating mental state, making daily life a continuous struggle.
Understanding these multifaceted impacts underscores the urgent need for accurate and comprehensive diagnosis, not just symptomatic treatment.
The Elusive Diagnosis: Why "Lfs Krankheit" Remains a Mystery
One of the biggest hurdles in effectively treating sleep disorders is the inherent difficulty in achieving a precise diagnosis. Unlike many other medical conditions with clear biomarkers, sleep issues often present a complex web of subjective symptoms and subtle physiological changes.
General practitioners (GPs) are typically the first point of contact for patients struggling with sleep. However, their diagnostic toolkit is often limited. Relying primarily on patient anamnesis – a diagnostic method based on a patient's self-reported history – presents significant challenges:
- Time Constraints: Busy GPs often lack the time required for a thorough, in-depth exploration of a patient's sleep patterns, lifestyle, and potential contributing factors.
- Subjective Patient Data: Patient accounts can be unreliable. What one person describes as "poor sleep" might differ vastly from another's experience, and recall bias can skew perceptions of sleep duration and quality.
More recent alternatives like actigraphs (sleep protocols worn on the wrist) can offer some objective data, but their utility is also restricted. While they can register restless sleep or periods of activity, they cannot provide a comprehensive picture of sleep stages, apneas, or other underlying physiological disturbances crucial for a definitive diagnosis of many forms of
Lfs Krankheit.
For truly complex diagnoses, specialized sleep medicine centers are indispensable. These facilities employ an objective complex method known as
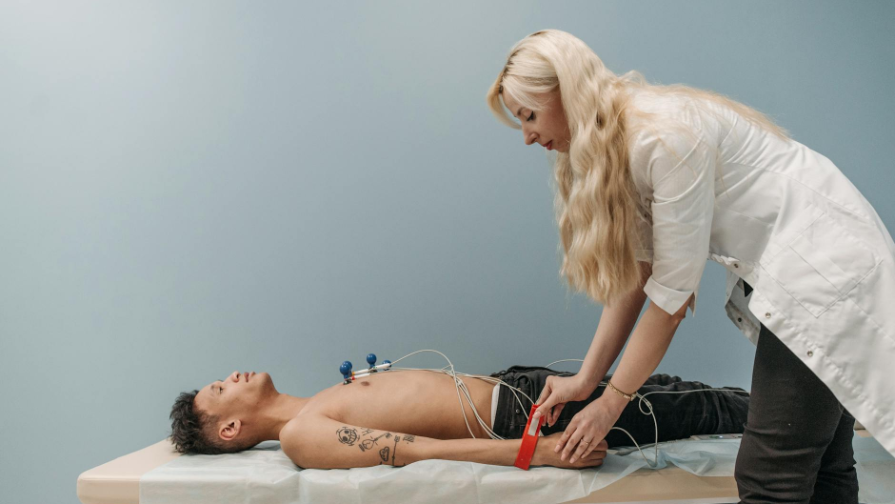
Electrophysiological Sleep Polygraphy – commonly referred to as a sleep study or polysomnography. During this overnight assessment, various physiological parameters are monitored, including:
- Brain activity (EEG)
- Eye movements (EOG)
- Muscle activity (EMG)
- Heart rate (ECG)
- Breathing patterns and oxygen levels
This intricate data allows specialists to differentiate between various sleep disorders, such as obstructive sleep apnea, restless legs syndrome, narcolepsy, and specific types of insomnia. Additionally, specialized clinics (neurology/psychiatry) utilize psychodiagnostic methods for insomnia, though these too often rely heavily on subjective data, albeit with expert interpretation.
The stark contrast between the diagnostic capabilities of a GP and a specialized sleep clinic highlights a critical flaw in the current healthcare model. The average general practitioner simply lacks the comprehensive diagnostic aids to make truly differentiated diagnostic or therapeutic statements regarding sleep disorders. This fundamental gap often leaves patients with an undiagnosed
Lfs Krankheit, vulnerable to generalized and potentially inappropriate treatments. For a deeper dive into these diagnostic challenges, consider reading
LFS Krankheit: The Hidden Flaws in Sleep Disorder Diagnosis.
The Risky Prescription Paradox: When Medication Outpaces Diagnosis
Given the diagnostic limitations at the primary care level, it's perhaps unsurprising that medication prescriptions for sleep disorders are often of "very doubtful value." Studies from Fischer (1967) and Frey and Gensch (1989) indicated that approximately 40-50% of patients consult a general practitioner for their sleep disturbances. This staggering figure underscores the immense responsibility placed on GPs regarding diagnosis and therapy.
However, the current reality often sees medication prescribed in what can only be described as a "diametral relationship" to the quality of the diagnosis. Without robust diagnostic tools, GPs are often forced to treat symptoms rather than root causes. This approach carries significant risks:
- Masking Underlying Conditions: Sedatives or hypnotics might induce sleep, but they do nothing to address conditions like sleep apnea, which can have life-threatening consequences if left untreated.
- Dependency and Side Effects: Many sleep medications carry risks of dependency, tolerance, and withdrawal symptoms. They can also have a range of undesirable side effects, including daytime grogginess, impaired cognitive function, and increased risk of falls, especially in older adults.
- Inappropriate Treatment: Prescribing medication for a sleep disorder that could be better managed with behavioral therapies, lifestyle changes, or specific medical devices (like CPAP for apnea) not only delays effective treatment but can also compound the patient's problems.
This reliance on pharmacological solutions without a secure diagnosis goes against the fundamental medical principle of "first, do no harm," emphasizing the urgent need for a more structured and evidence-based approach to an
Lfs Krankheit.
Navigating the Path to Accurate Diagnosis and Treatment
For individuals suspecting they suffer from a sleep disorder, taking proactive steps is crucial. The key lies in understanding that not all medical professionals are equally equipped to diagnose and manage complex sleep conditions.
*
Seek Specialized Care: If your sleep issues are chronic (GPs often define chronic as occurring 3 or more nights a week for an extended period) or significantly impacting your daily life, advocate for a referral to a sleep medicine specialist or clinic. These centers possess the expertise and technology to conduct comprehensive evaluations like polysomnography.
*
Keep a Detailed Sleep Diary: Before any consultation, maintain a meticulous sleep diary for at least two weeks. Record:
- Bedtime and wake-up time
- Time taken to fall asleep
- Number and duration of awakenings
- Subjective sleep quality
- Any daytime symptoms (fatigue, irritability)
- Consumption of caffeine, alcohol, or medications
- Any significant events or stressors
This objective data can provide invaluable insights for specialists.
*
Explore Behavioral Therapies: For many forms of insomnia, Cognitive Behavioral Therapy for Insomnia (CBT-I) is considered the first-line treatment. CBT-I addresses the thoughts, feelings, and behaviors that contribute to sleep problems without the risks associated with medication. It's a highly effective, non-pharmacological approach that can provide long-term relief.
*
Understand the Interdisciplinary Approach: Effective treatment of an
Lfs Krankheit often involves a team approach, including sleep physicians, neurologists, psychiatrists, psychologists, and sometimes dentists (for oral appliances in sleep apnea). This holistic perspective ensures that all contributing factors are considered. To discover more about the specialized avenues available, explore
Beyond the GP: Uncovering True Sleep Disorder Diagnostics.
Conclusion
The journey from chronic sleeplessness to restful nights is often fraught with diagnostic challenges and the temptation of quick-fix medications. The critical distinction between highly specialized sleep medical clinics and general practitioners' capabilities highlights a systemic issue where the secure diagnosis, a cornerstone of medical practice, is often bypassed. Recognizing the profound impact of an undiagnosed
Lfs Krankheit on physical, mental, and social well-being is the first step. By empowering ourselves with knowledge, advocating for thorough diagnostic processes, and exploring specialized and holistic treatment options, we can move towards a healthcare system that prioritizes accurate diagnosis over risky, generalized prescriptions, ultimately leading to healthier, more rested lives.